Dental Implant Materials Guide: Titanium, Zirconia, Abutments
Choosing implant materials is more than a cosmetic decision: it can influence healing, long-term stability, and how natural a replacement tooth looks and feels. This guide explains titanium and zirconia implants, common abutment materials, and how these parts work together so Canadian patients can have clearer conversations with their dental team.
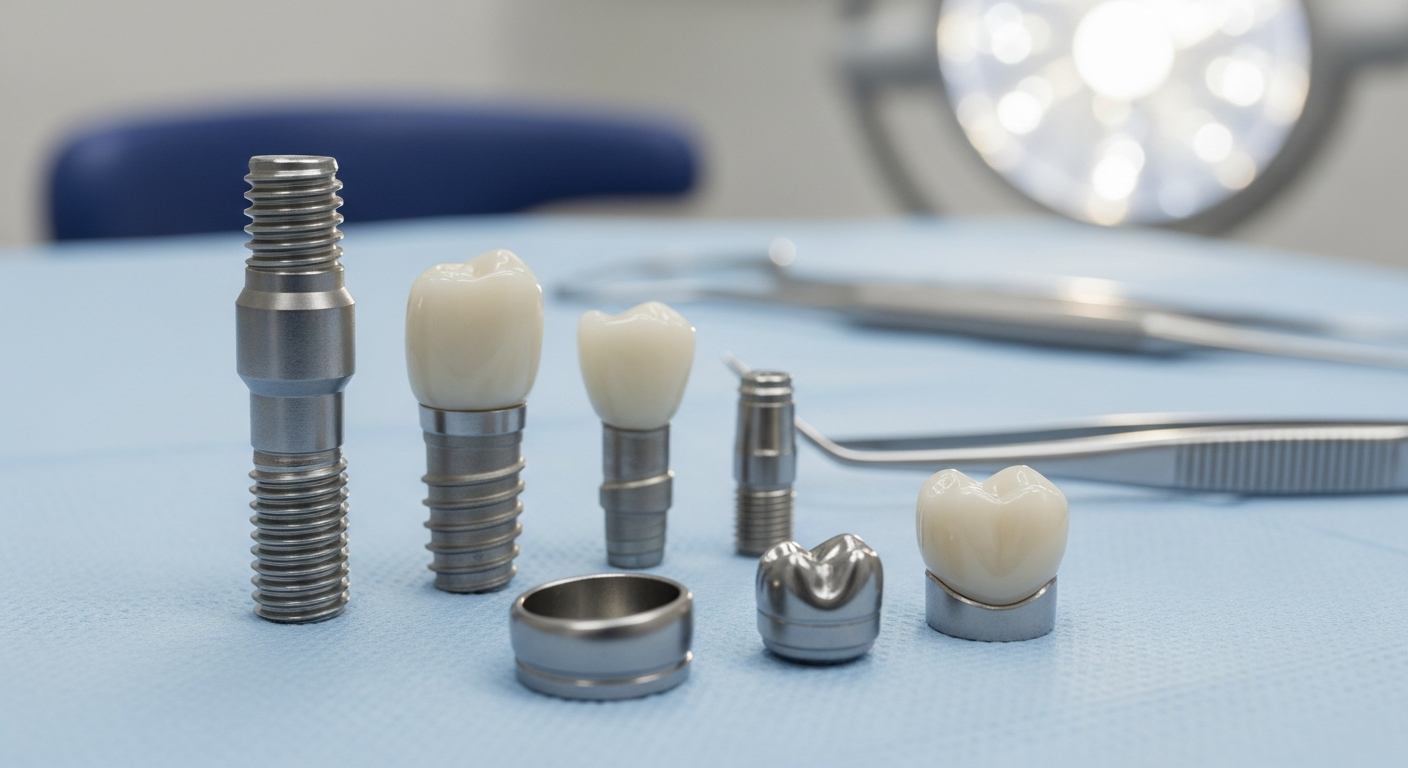
Material choices sit at the center of how an implant-supported tooth is planned, placed, and restored. Even when two treatments look identical from the outside, the underlying metals or ceramics, the implant–abutment connection, and the crown interface can differ in ways that affect strength, hygiene, and aesthetics. The overview below breaks down the main options you may hear about in Canada.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Guide to Dental Implants: parts and material roles
A typical implant system has three functional layers: the implant fixture (the post placed into the jaw), the abutment (the connector), and the final restoration (often a crown). The fixture is designed for osseointegration, the biological bonding between bone and the implant surface. Its material must be biocompatible, corrosion-resistant, and strong under repeated chewing forces.
The abutment sits at or above the gumline, so its material can influence soft-tissue response and how much grey shadowing shows through thin gums. The crown material (such as porcelain-fused-to-metal or all-ceramic) mainly affects appearance and wear against opposing teeth, but it also interacts with the abutment via cement or a screw channel. When people ask for a Guide to Dental Implants, it often helps to separate these roles: the fixture is about integration and load; the abutment is about the gum interface and fit; the crown is about function and appearance.
2026 Dental Implants Guide: titanium vs zirconia
Titanium remains the most commonly used implant fixture material because it has a long clinical track record, high strength-to-weight ratio, and excellent corrosion resistance in the oral environment. Many systems use commercially pure titanium or titanium alloys; the precise formulation varies by manufacturer. Surface characteristics also matter: moderately roughened surfaces can support bone response, but they also require good hygiene and professional maintenance to reduce the risk of plaque-related inflammation.
Zirconia implants are made from a high-strength ceramic (zirconium dioxide). One reason patients ask about zirconia is aesthetics: a tooth-coloured fixture may reduce the chance of a grey hue near the gumline in thin tissue. Zirconia is also metal-free, which some patients prefer. Trade-offs are more nuanced: zirconia behaves differently under stress than titanium, and the design options may be more limited depending on the system (for example, one-piece designs that combine implant and abutment can reduce micro-movement at a junction but may restrict restorative flexibility and angle correction).
For a practical 2026 Dental Implants Guide discussion with your clinician, ask how your gum thickness, bite forces (such as clenching or grinding), available bone, and aesthetic priorities affect material choice. In many plans, surgical factors (bone volume and implant position) and maintenance factors (your ability to clean around the restoration and attend recalls) matter as much as the base material.
Technical Guide: Dental Implants, abutments and connections
Abutments are commonly titanium, zirconia, or (less often today) gold-coloured alloys; some cases also use high-performance polymers as temporary or specialized components. Titanium abutments are valued for strength and a precise fit with many implant connections. Zirconia abutments can improve appearance in the aesthetic zone, especially with thin gums, but they are typically used with careful attention to design thickness and load direction.
Connection design affects how the implant and abutment meet. You may hear terms such as internal hex, conical (Morse taper), or external connections. The goal is a stable interface that resists loosening and limits micro-gaps where bacteria can colonize. No connection eliminates biological risk on its own; inflammation around implants (often discussed as peri-implant mucositis or peri-implantitis) is multifactorial and strongly linked to plaque control, smoking status, history of gum disease, and regular professional monitoring.
Restorations can be screw-retained or cement-retained. Screw-retained crowns often make retrievability easier for maintenance or repairs, while cement-retained crowns can be useful in certain aesthetic or space-limited situations but require meticulous cement removal to reduce irritation. If you are comparing technical options, a Technical Guide: Dental Implants conversation typically includes: abutment material, connection type, crown retention method, and how the clinic will verify fit (digital scans, radiographs, torque protocols, and follow-up checks).
Choosing between titanium and zirconia is rarely a single yes-or-no decision. Many successful plans combine materials, such as a titanium fixture with a zirconia abutment and an all-ceramic crown, or a titanium fixture with a titanium abutment where strength and durability are the priority. The most helpful questions are usually case-specific: how will the material look through my gum tissue, how will it handle my bite, what maintenance is required, and what signs of complications should I watch for between recall visits.