Safety Checks Dermatologists Use for Dark Lip Laser Procedures
Darkened lips can have many causes, from post-inflammatory pigmentation to smoking, sun exposure, or irritation from cosmetics. Because the lip area is thin, vascular, and highly reactive, dermatologists typically rely on structured safety checks before considering laser-based pigment removal. Understanding these checks helps set realistic expectations and reduce avoidable risks.
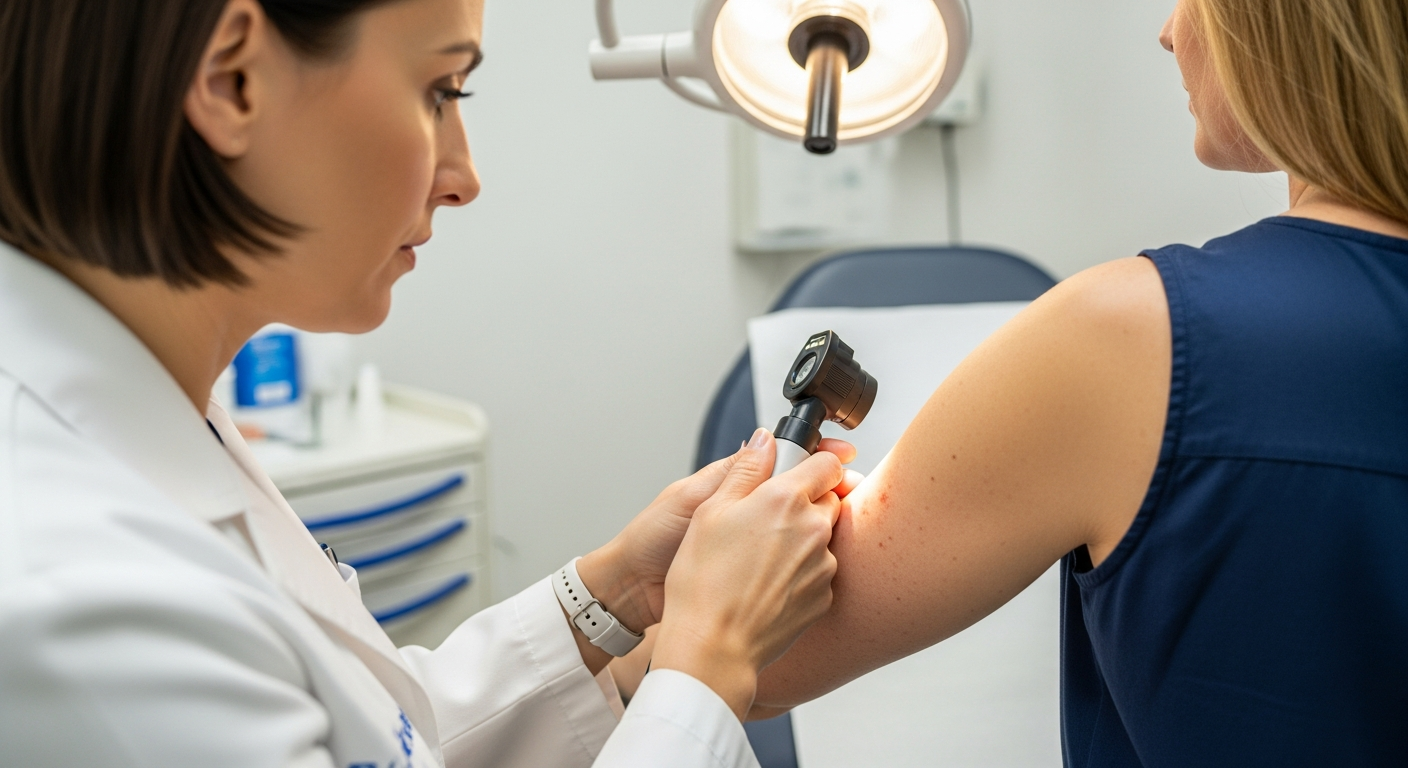
The lips behave differently from other facial skin: the barrier is thinner, pigment can sit at varying depths, and irritation can quickly trigger more discoloration. In Singapore, where daily UV exposure is common and many patients have medium-to-deeper skin tones, dermatologists usually take extra steps to reduce the chance of burns, scarring, or rebound pigmentation before any laser procedure is considered.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
How laser treatment for dark lips is approached in clinical practice
A dermatologist typically starts by confirming that “dark lips” are due to pigment rather than circulation-related colour changes, dryness, or active inflammation. Common clinical questions include when the darkening started, whether it fluctuates, and whether it is limited to the lip border or involves the inner lip (mucosa), since the latter may change which treatments are appropriate.
A detailed exposure history is also a safety check. Clinicians often ask about smoking or vaping, lip-licking habits, frequent use of matte or long-wear products, fragranced balms, and recent lip procedures. Prior reactions to lip products can suggest allergic contact dermatitis, where controlling inflammation is usually prioritised because lasers applied to irritated skin can increase the risk of post-inflammatory hyperpigmentation.
Medication and health screening matters as well. Dermatologists commonly review recent isotretinoin use, photosensitising medicines, anticoagulants, history of keloid or hypertrophic scars, and a tendency toward cold sores. Even when laser is technically feasible, a plan may include stabilising the skin first and addressing triggers that could keep re-darkening the lips after treatment.
How laser treatment for dark lips is evaluated in dermatology care
Before selecting a device, dermatologists evaluate skin tone and pigment behaviour. A common framework is assessing the patient’s tendency to tan or develop hyperpigmentation after irritation (often correlated with Fitzpatrick skin type, which is frequently III–V in Singapore). This affects how conservative settings may be and how strongly pre- and post-care is emphasised.
They also assess the likely depth and pattern of pigment. Diffuse, soft-edged darkening after chronic irritation may respond differently than sharply demarcated pigmentation along the vermilion border. If the appearance suggests a medical condition, a clinician may recommend further assessment rather than proceeding directly with cosmetic laser treatment.
Patch testing or test-spotting is a practical safety check many clinics use for higher-risk skin types or uncertain cases. A small-area test can help gauge how the lip tissue responds, whether swelling is excessive, and whether there is early evidence of unwanted lightening, blistering, or darkening. Because pigment changes can take time to declare themselves, the assessment may include waiting days to weeks before a full treatment.
Eye protection and infection control are also part of clinical evaluation, not an afterthought. The lips are close to the eyes and frequently exposed to saliva and bacteria, so dermatology protocols often include laser-specific protective eyewear, strict device hygiene, and guidance to avoid treating over broken skin or active infections.
What laser treatment for dark lips involves in treatment planning
When laser is considered appropriate, planning usually focuses on matching the laser type and settings to pigment depth while minimising heat injury. Dermatologists may use pigment-targeting approaches (often in the category of Q-switched or picosecond platforms for certain pigment issues) or other modalities depending on the diagnosis and tissue characteristics. The exact device choice and parameters are typically individualised rather than “one size fits all.”
A safety-first plan also includes pain control and swelling management. Cooling methods, topical anaesthesia when appropriate, and careful spacing of pulses can reduce discomfort and lower the risk of overtreatment. Because lip tissue can swell quickly, clinicians may treat in smaller zones and reassess frequently during the session.
Pre-treatment preparation commonly includes reducing avoidable irritants. A dermatologist may advise pausing new cosmetics, avoiding lip exfoliants, and controlling dryness beforehand. If there is a known history of herpes simplex outbreaks, some clinicians consider preventive strategies based on individual risk, because procedures around the mouth can trigger flare-ups and complicate healing.
Aftercare planning is a major safety checkpoint because the lip area is constantly exposed to food, drinks, and friction. Typical guidance may include gentle cleansing, avoidance of picking or aggressive rubbing, sun protection habits (including physical barriers like hats and shade), and monitoring for warning signs such as increasing pain, blistering, spreading redness, pus, or fever. Follow-up timing is often scheduled to detect early pigment rebound, uneven lightening, or delayed irritation.
Finally, dermatologists usually discuss realistic outcomes and boundaries. Some lip colour variation is normal due to blood vessels and natural melanin distribution, and overly aggressive treatment can cause textural change or unwanted lightening. For that reason, many treatment plans are incremental, with reassessment between sessions and a willingness to stop or switch strategies if the risk-benefit balance changes.
In practice, safe dark lip laser care is less about the “laser session” and more about the checks around it: confirming the cause, evaluating pigment risk, choosing conservative parameters, and supporting healing. These steps help reduce preventable complications and improve the chance that any brightening achieved is even, stable, and compatible with the patient’s natural lip tone.




